MedicalMex – Social Reviews & Recommendations
The Best Medical Procedures in Mexico
Gastric Sleeve Surgery Patient Rreview
MedicalMex is the #1 option for weight loss surgery in Mexico
The Weight Loss Surgery of Angel from New Zealand.
My experience WLS with MedicalMex
Thank you so much Timmie for the words, energy and support!
Thank you so much Edith for sharing your WLS experience!
Best Gastric Sleeve Surgeon in Tijuana, Mexico
MedicalMex, The Safe, Affordable and Personalized Experience
- US and Mexico Board Certified Weight Loss Surgeon
- Personalized Experience, unlike everywhere else, we only accept one Weight Loss Surgery per day to ensure the highest level of personalized care from our entire team caring for your wellbeing and satisfaction
- Home to Dr. Russell Fok a trusted name in Weight-loss Surgery
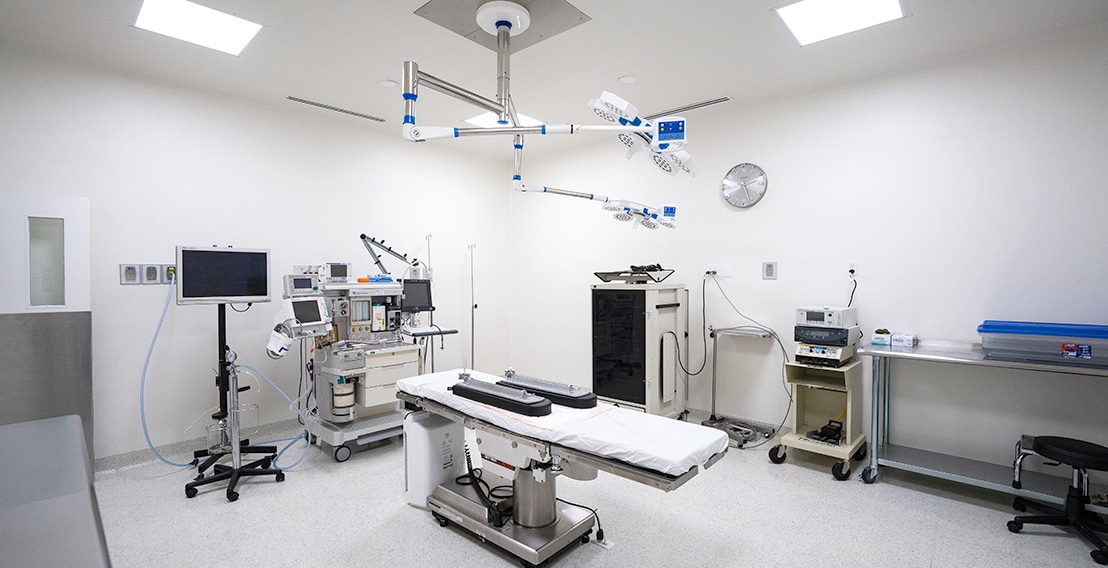
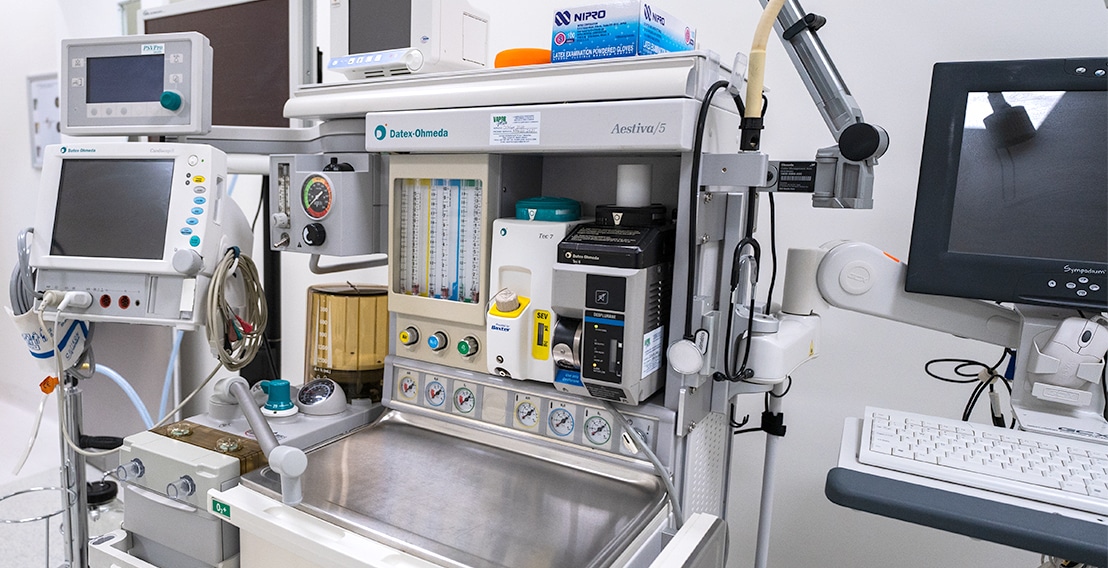
- Full-scale certified hospitals and clinics with International Accreditation’s
- Best technologically advanced medical facilities in Tijuana
- Personal Transportation Services
- Concierge Services for Any Type of Additional Needs
- Comfortable rooms with space available for companion upon request
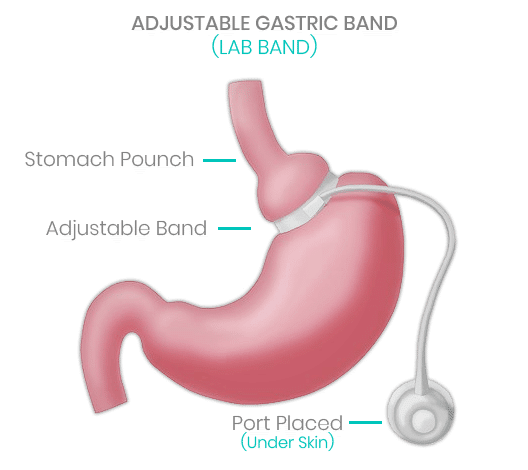
Gastric Band Surgery (Lap-Band)
Gastric Band Surgery Price $ 5,600 USD
The Gastric Band surgery (Gastric Banding), also known as lap-band surgery involves placing a band around the stomach which makes it function as though it was smaller. Unlike other weight-loss surgery procedures, the lap-band can be adjusted to decrease or increase food digestion and it can be removed later on the patient chooses too.
Don’t risk it, go with the safest option for you land-band surgery in Mexico.
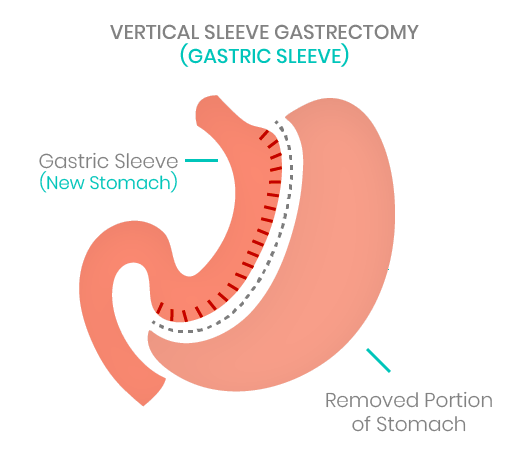
Gastric Sleeve Surgery (Vertical Sleeve Gastrectomy VSG)
Gastric Sleeve Surgery Price: $4,600 USD
The Gastric Sleeve surgery, also known as Vertical Sleeve Gastrectomy or VSG surgery is one of the most popular approaches for long-term weight loss. The VSG surgery woks similar to the bypass surgery, the process involves shrinking the stomach, only this time a section of the stomach is removed and replaced with a sleeve or banana-shaped tube. The VSG surgery is a relatively new form of weight-loss surgery that has gained huge popularity in recent years as it has proven a great alternative to laparoscopic gastric band surgery.
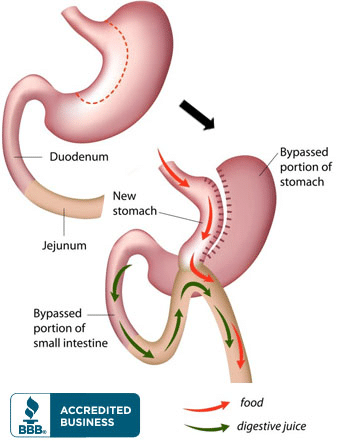
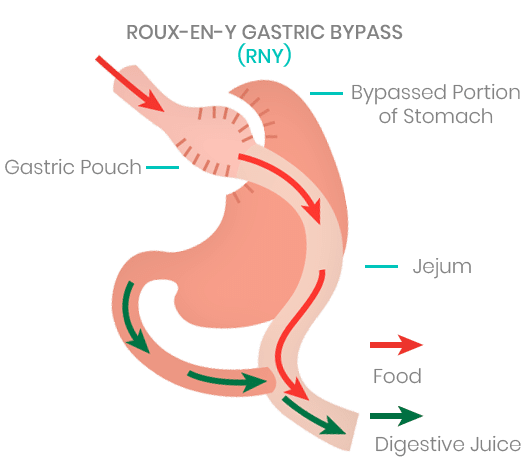
Gastric Bypass Surgery (Roux-en-Y)
Gastric Bypass Surgery Price: $5,500 usd
The Gastric Bypass or Roux-en-Y surgery is also another very popular and effective long-term weight loss solution, it involves “splitting” the stomach into two parts. The upper-most section, measures only an inch or so in diameter, and is the only part that will collect the food, bypassing the lower region of the stomach and the the small intestine, thus reducing the amount of calories absorbed to produce the weight-loss. Gastric Bypass expenses can cost up to $40,000 in some US hospital but with us, you get Dr. Pablo Fok Russell the leading weight-loss surgeon in Mexico, the best and only certified medical facilities and the only place to offer US based case manager to help every step along the way for a small fraction of the cost. Don’t risk it, go with the safest option for you Bypass surgery in Mexico.
Bariatric Revision Surgery (Body Contouring)
Bariatric Revision Surgery Price: Varies by patient
The Revision Bariatric weight-loss surgery is intervention too repair or revise a prior weight-loss surgical procedure. This can be patients that were not successful with their prior procedure, or patients with partial success but that want to improve or remove sagging skin from the massive weigh-loss. The weight-loss revision surgery is the specialty of Dr. Pablo Fok Russell who for over 17 years has mentor and trained many surgeons on best practices and better techniques for weight-loss surgery, making him the natural option for best bariatric revision surgery in Mexico.

Mini Gastric Bypass Surgery (MGB)
Our Price: $ 5,500 USD
Our Mini Gastric Bypass Surgery (MGB) is a laparoscopic, mal-absorptive and restrictive bariatric procedure which makes our patients feel full sooner, absorb fewer calories and it’s one of the few weight loss surgeries that can be revised and reversible.